US coronavirus cases approach 9 million with no end in sight | ABS-CBN
ADVERTISEMENT

Welcome, Kapamilya! We use cookies to improve your browsing experience. Continuing to use this site means you agree to our use of cookies. Tell me more!
US coronavirus cases approach 9 million with no end in sight
US coronavirus cases approach 9 million with no end in sight
Mitch Smith,
Simon Romero and Giulia McDonnell Nieto del Rio,
The New York Times
Published Oct 30, 2020 06:55 AM PHT
|
Updated Oct 30, 2020 08:31 AM PHT
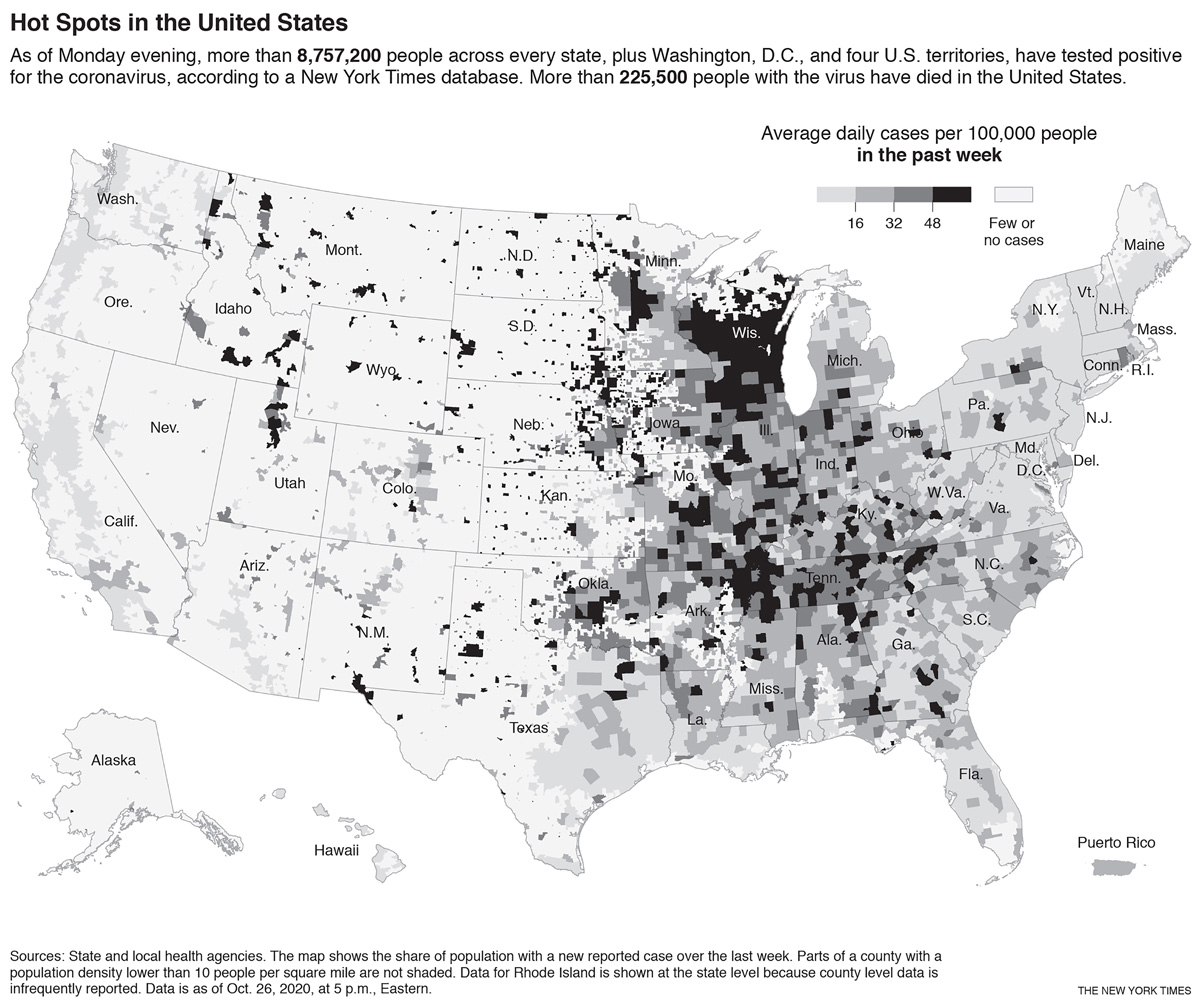
CHICAGO — The United States, which reported one of its earliest coronavirus cases in Washington state in the beginning of the year, approached more than 9 million total infections Thursday, including more than half a million in the past week, as the virus spiraled out of control in the lead up to Election Day.
CHICAGO — The United States, which reported one of its earliest coronavirus cases in Washington state in the beginning of the year, approached more than 9 million total infections Thursday, including more than half a million in the past week, as the virus spiraled out of control in the lead up to Election Day.
Across the country, alarming signs suggested the worst was yet to come: More than 20 states reported more cases over the past week than at any time during the pandemic. Patients were sent to field hospitals in El Paso, Texas, and the Milwaukee suburbs. Growing outbreaks led to new restrictions on businesses in Chicago. Zero states reported sustained declines in cases.
Across the country, alarming signs suggested the worst was yet to come: More than 20 states reported more cases over the past week than at any time during the pandemic. Patients were sent to field hospitals in El Paso, Texas, and the Milwaukee suburbs. Growing outbreaks led to new restrictions on businesses in Chicago. Zero states reported sustained declines in cases.
“There is no way to sugarcoat it — we are facing an urgent crisis, and there is an imminent risk to you, your family members, your friends, your neighbors,” said Gov. Tony Evers of Wisconsin, where hospitals have been strained, case numbers have exploded and more than 200 coronavirus deaths have been announced in the past week.
“There is no way to sugarcoat it — we are facing an urgent crisis, and there is an imminent risk to you, your family members, your friends, your neighbors,” said Gov. Tony Evers of Wisconsin, where hospitals have been strained, case numbers have exploded and more than 200 coronavirus deaths have been announced in the past week.
With the presidential election days away, the country is now averaging more than 75,000 new cases daily, the worst stretch of the pandemic by that measure. Deaths, which lag behind cases, remain far below their spring levels but have ticked upward to about 780 each day. More cases have been identified in the United States than in any other country, though some nations have higher per capita infection rates.
With the presidential election days away, the country is now averaging more than 75,000 new cases daily, the worst stretch of the pandemic by that measure. Deaths, which lag behind cases, remain far below their spring levels but have ticked upward to about 780 each day. More cases have been identified in the United States than in any other country, though some nations have higher per capita infection rates.
ADVERTISEMENT
“This surge is larger than any other wave or surges that we’ve seen yet,” said Amanda Simanek, an epidemiologist at the University of Wisconsin-Milwaukee school of public health, who said she was especially worried to see case numbers spiking just as colder weather forces more people indoors, where the virus can spread easily. “This is the pattern that may continue to happen if we don’t suppress the infection down to levels that are manageable.”
“This surge is larger than any other wave or surges that we’ve seen yet,” said Amanda Simanek, an epidemiologist at the University of Wisconsin-Milwaukee school of public health, who said she was especially worried to see case numbers spiking just as colder weather forces more people indoors, where the virus can spread easily. “This is the pattern that may continue to happen if we don’t suppress the infection down to levels that are manageable.”
Recent data is almost uniformly grim.
Recent data is almost uniformly grim.
Twenty-one states added more cases in the seven-day period ending Wednesday than in any other seven-day stretch of the pandemic. In parts of Idaho and Kansas, officials have warned that few hospital beds remained. In North Dakota, where more than 5% of the population has now tested positive, case numbers continue to soar, with a single-day record of more than 1,200 new infections Thursday. As the country approached 9 million cases, experts lamented opportunities lost that might have limited the spread.
Twenty-one states added more cases in the seven-day period ending Wednesday than in any other seven-day stretch of the pandemic. In parts of Idaho and Kansas, officials have warned that few hospital beds remained. In North Dakota, where more than 5% of the population has now tested positive, case numbers continue to soar, with a single-day record of more than 1,200 new infections Thursday. As the country approached 9 million cases, experts lamented opportunities lost that might have limited the spread.
“I think it’s surprising how quickly it happened,” said Dr. Larry Chang, an infectious-disease expert at Johns Hopkins University School of Medicine. “I thought we would do a better job as a country getting organized and coming up with evidence-based national plans for mitigating this epidemic. So, while I’m not surprised we reached this number, it happened a lot faster than I thought it would.”
“I think it’s surprising how quickly it happened,” said Dr. Larry Chang, an infectious-disease expert at Johns Hopkins University School of Medicine. “I thought we would do a better job as a country getting organized and coming up with evidence-based national plans for mitigating this epidemic. So, while I’m not surprised we reached this number, it happened a lot faster than I thought it would.”
The latest national uptick started weeks ago in the Upper Midwest and the Mountain West but has now spread far beyond those regions. In the Northeast, places like New Jersey and Rhode Island have seen rising infection numbers after months of stability. Kentucky and Pennsylvania are among the states seeing record case numbers. And in Texas, the situation around El Paso is so dire that officials have ordered a curfew, and some coronavirus patients have had to be flown elsewhere.
The latest national uptick started weeks ago in the Upper Midwest and the Mountain West but has now spread far beyond those regions. In the Northeast, places like New Jersey and Rhode Island have seen rising infection numbers after months of stability. Kentucky and Pennsylvania are among the states seeing record case numbers. And in Texas, the situation around El Paso is so dire that officials have ordered a curfew, and some coronavirus patients have had to be flown elsewhere.
All the while, there was a sense that concerns about the health risks have quieted since the early days of the virus when lockdown orders were widespread. Businesses remain open in much of the country. Many students continue to attend classes. There is no national mask mandate. And President Donald Trump, who has spoken hopefully about a vaccine, has insisted to large campaign rally crowds that the country is “rounding the corner.”
All the while, there was a sense that concerns about the health risks have quieted since the early days of the virus when lockdown orders were widespread. Businesses remain open in much of the country. Many students continue to attend classes. There is no national mask mandate. And President Donald Trump, who has spoken hopefully about a vaccine, has insisted to large campaign rally crowds that the country is “rounding the corner.”
“This was preventable,” said Kaitlyn Urenda-Culpepper, whose mother died from the coronavirus this summer in El Paso and who said she was frustrated by the state and federal response as her “hometown is getting ransacked.” She said, “My mother did not have to die.”
“This was preventable,” said Kaitlyn Urenda-Culpepper, whose mother died from the coronavirus this summer in El Paso and who said she was frustrated by the state and federal response as her “hometown is getting ransacked.” She said, “My mother did not have to die.”
Back in the spring — when testing was limited, protective gear was scarce and the country at times averaged more than 2,000 deaths per day — the worst of the pandemic was concentrated in big cities in the Northeast. This summer, when case numbers spiked to an average of more than 66,000 per day, the Sun Belt suffered most. Now, despite increased testing and improved medical care, the rapidly growing outbreaks have spread across regional lines and strained hospitals in big cities and small towns alike.
Back in the spring — when testing was limited, protective gear was scarce and the country at times averaged more than 2,000 deaths per day — the worst of the pandemic was concentrated in big cities in the Northeast. This summer, when case numbers spiked to an average of more than 66,000 per day, the Sun Belt suffered most. Now, despite increased testing and improved medical care, the rapidly growing outbreaks have spread across regional lines and strained hospitals in big cities and small towns alike.
“My biggest concern is not having the staff for the beds we’re opening up,” said Dani Beebe, a nurse in an intensive care unit at Intermountain Medical Center in Murray, Utah. “We’re already looking at a future reality where every physician we have is caring for COVID patients regardless of their specialty.”
“My biggest concern is not having the staff for the beds we’re opening up,” said Dani Beebe, a nurse in an intensive care unit at Intermountain Medical Center in Murray, Utah. “We’re already looking at a future reality where every physician we have is caring for COVID patients regardless of their specialty.”
Beebe said that health workers had learned a great deal about strategies for caring for COVID-19 patients since the start of the pandemic but that “it’s definitely worse now” because of the growing number of hospitalizations.
Beebe said that health workers had learned a great deal about strategies for caring for COVID-19 patients since the start of the pandemic but that “it’s definitely worse now” because of the growing number of hospitalizations.
“We’re preparing our surge plans, but people are already dying,” Beebe said. “You think they’re improving, and a day later they’re fighting for their lives or needing care for weeks on end.”
“We’re preparing our surge plans, but people are already dying,” Beebe said. “You think they’re improving, and a day later they’re fighting for their lives or needing care for weeks on end.”
Catherine Troisi, an infectious-disease epidemiologist at the University of Texas Health Science Center at Houston, said the country’s response had been hampered by politicians declining to follow the recommendations of health officials.
Catherine Troisi, an infectious-disease epidemiologist at the University of Texas Health Science Center at Houston, said the country’s response had been hampered by politicians declining to follow the recommendations of health officials.
“We have pandemic fatigue; everybody’s sick of this, right?” Troisi said. “But you know what, the virus doesn’t care.”
“We have pandemic fatigue; everybody’s sick of this, right?” Troisi said. “But you know what, the virus doesn’t care.”
© 2020 The New York Times Company
Read More:
United States
COVID-19
coronavirus
infection
deaths
death toll
united states coronavirus
coronavirus united states
new york times
coronavirus surge
ADVERTISEMENT
ADVERTISEMENT