‘Ang daming love from everyone’: Young MD who survived COVID-19 recalls struggle, then hope | ABS-CBN

Welcome, Kapamilya! We use cookies to improve your browsing experience. Continuing to use this site means you agree to our use of cookies. Tell me more!
‘Ang daming love from everyone’: Young MD who survived COVID-19 recalls struggle, then hope
‘Ang daming love from everyone’: Young MD who survived COVID-19 recalls struggle, then hope
Kristine Sabillo,
ABS-CBN News
Published Apr 28, 2020 09:55 PM PHT
|
Updated Apr 28, 2020 11:24 PM PHT
MANILA—At 26 years old, Dr. Carmina Fuentebella has a lot to look forward to. She wanted to travel, be a great doctor and have her own family.
MANILA—At 26 years old, Dr. Carmina Fuentebella has a lot to look forward to. She wanted to travel, be a great doctor and have her own family.
These were exactly her thoughts when she suddenly became severely sick from COVID-19 and on the brink of death.
These were exactly her thoughts when she suddenly became severely sick from COVID-19 and on the brink of death.
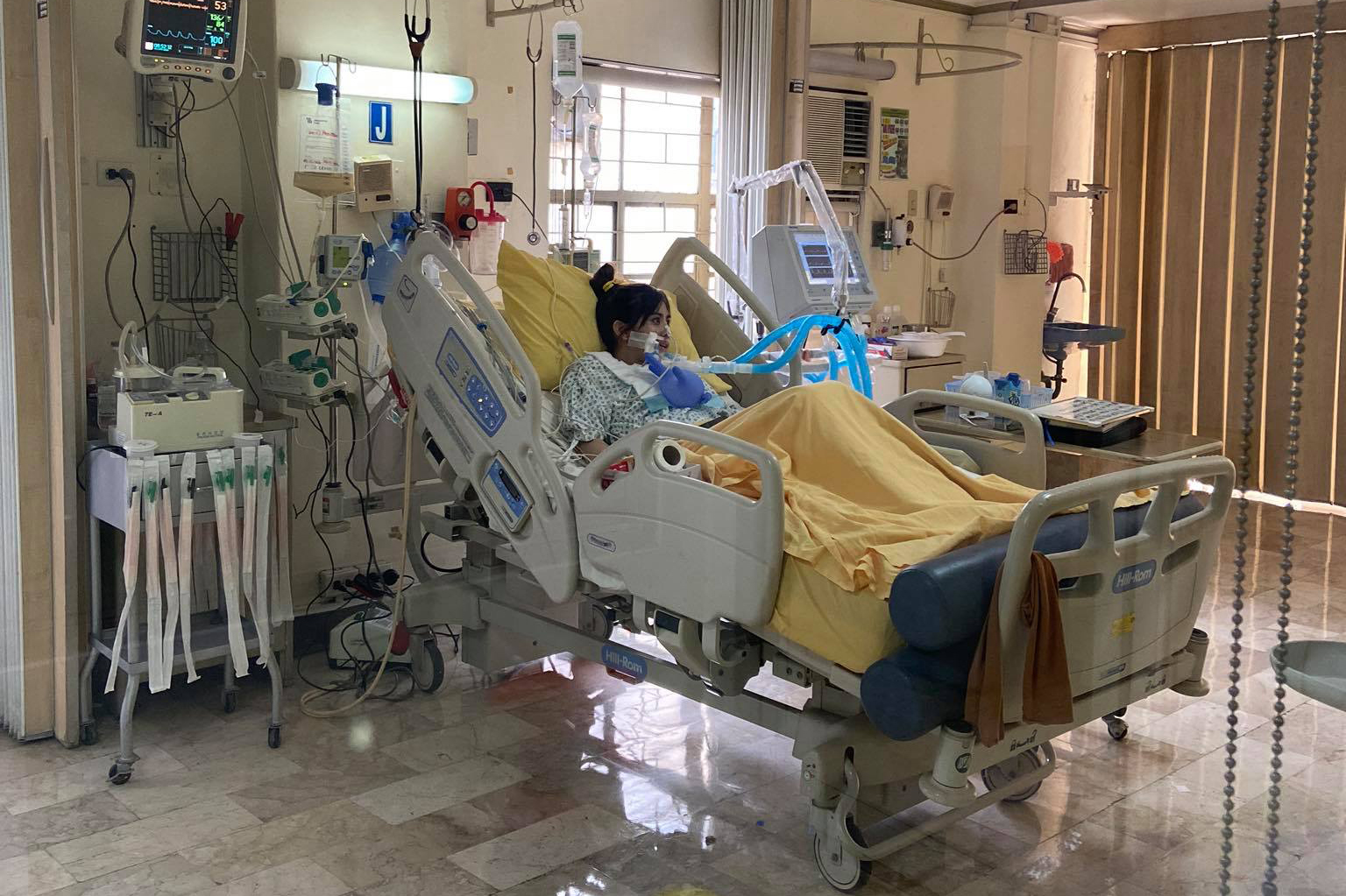
She was in intensive care, breathing through a mechanical ventilator, and under a lot of pain.
She was in intensive care, breathing through a mechanical ventilator, and under a lot of pain.
It was on April 4 that she felt her first symptom — body pain.
It was on April 4 that she felt her first symptom — body pain.
ADVERTISEMENT
“I thought it was just muscle strain since I was doing laundry the day before,” she told ABS-CBN News. But then she lost her appetite and felt too exhausted to leave the bed.
“I thought it was just muscle strain since I was doing laundry the day before,” she told ABS-CBN News. But then she lost her appetite and felt too exhausted to leave the bed.
“I had fever. I knew I was immediately (a) suspect COVID-19 case since I was handling a lot of patients who were probable and confirmed COVID19 cases.”
“I had fever. I knew I was immediately (a) suspect COVID-19 case since I was handling a lot of patients who were probable and confirmed COVID19 cases.”
For the last couple of months, Fuentebella, an internal medicine resident physician, had been managing suspected COVID-19 cases at the emergency room of University of Santo Tomas Hospital.
For the last couple of months, Fuentebella, an internal medicine resident physician, had been managing suspected COVID-19 cases at the emergency room of University of Santo Tomas Hospital.
She knew there was a risk of contracting the disease but she did not expect it to hit her hard.
She knew there was a risk of contracting the disease but she did not expect it to hit her hard.
After experiencing high fever and shortness of breath, she was admitted to the hospital. Her x-ray results showed that she had pneumonia.
After experiencing high fever and shortness of breath, she was admitted to the hospital. Her x-ray results showed that she had pneumonia.
Her condition deteriorated and on the third day she was intubated and hooked to a mechanical ventilator.
Her condition deteriorated and on the third day she was intubated and hooked to a mechanical ventilator.
“I was surprised because it’s not common (for a young person to experience such severe symptoms),” she said.
“I was surprised because it’s not common (for a young person to experience such severe symptoms),” she said.
Fuentebella said that except for allergies she did not have any pre-existing medical conditions. She was never confined at a hospital, even when she was a child.
Fuentebella said that except for allergies she did not have any pre-existing medical conditions. She was never confined at a hospital, even when she was a child.
GIVING UP
The young doctor said it came to a point when she just wanted to give up.
The young doctor said it came to a point when she just wanted to give up.
“Nu’ng una talaga ayoko na. Kasi nakakapagod s’ya. ’Yung tinutusok ka araw-araw. Hindi mo naiintindihan ’yung nangyayari sa’yo,” she said.
“Nu’ng una talaga ayoko na. Kasi nakakapagod s’ya. ’Yung tinutusok ka araw-araw. Hindi mo naiintindihan ’yung nangyayari sa’yo,” she said.
“Tapos nakatubo ka. Isa-suction ka pa. Hindi ’yan tubo lang. Aalisan ka ng plema, masusuka ka. Every day ’yun gagawin. Every four hours. Napakasakit nya.”
“Tapos nakatubo ka. Isa-suction ka pa. Hindi ’yan tubo lang. Aalisan ka ng plema, masusuka ka. Every day ’yun gagawin. Every four hours. Napakasakit nya.”
(I wanted to give up at first because it was wearing me out. They stick a needle in you everyday. You don’t understand what’s happening to you. Then you’re intubated, apply a suction on you, and it’s not just a tube. They extract your phlegm, you vomit. You do that everyday for four hours. It was really painful.)
(I wanted to give up at first because it was wearing me out. They stick a needle in you everyday. You don’t understand what’s happening to you. Then you’re intubated, apply a suction on you, and it’s not just a tube. They extract your phlegm, you vomit. You do that everyday for four hours. It was really painful.)
Fuentebella said she started telling her doctors to just remove the ventilator, because she was in so much pain.
Fuentebella said she started telling her doctors to just remove the ventilator, because she was in so much pain.
“Gusto ko pa mag-Japan nu’ng mga oras na iyon. Gusto ko maging magaling na doktor. Gusto ko maging nephrologist (specializing in kidney disease). Gusto ko pang magkapamilya kaso nga lang may point in life na ’pag nasasaktan ka talaga gusto mong mag-give up,” she acknowledged.
“Gusto ko pa mag-Japan nu’ng mga oras na iyon. Gusto ko maging magaling na doktor. Gusto ko maging nephrologist (specializing in kidney disease). Gusto ko pang magkapamilya kaso nga lang may point in life na ’pag nasasaktan ka talaga gusto mong mag-give up,” she acknowledged.
PRAYER BRIGADES
Little did she know that thousands of strangers were praying for her recovery after reading about her condition online.
Little did she know that thousands of strangers were praying for her recovery after reading about her condition online.
After spending more than a week at the hospital, her relatives posted her condition on social media, calling for people to pray for her. The posts went viral and soon many groups were calling on people to pray for her.
After spending more than a week at the hospital, her relatives posted her condition on social media, calling for people to pray for her. The posts went viral and soon many groups were calling on people to pray for her.
“Doon sa phone ko ang daming love from everyone talaga. Ang daming nagte-text sa akin. ‘Kamusta ka?’ ’Wag kang susuko,’ ” Fuentebella said.
“Doon sa phone ko ang daming love from everyone talaga. Ang daming nagte-text sa akin. ‘Kamusta ka?’ ’Wag kang susuko,’ ” Fuentebella said.
Her fellow health workers also started posting photos of her family and friends on the wall of her room.
Her fellow health workers also started posting photos of her family and friends on the wall of her room.
“Tapos every day kong tinitignan ’yon. ’Pag may mga oras na gusto kong mag-give up sisilipin ko ’yung pictures namin magkakasama tapos doon ko maiisip ko: kailangan ko na namang lumaban ngayon,” she said.
“Tapos every day kong tinitignan ’yon. ’Pag may mga oras na gusto kong mag-give up sisilipin ko ’yung pictures namin magkakasama tapos doon ko maiisip ko: kailangan ko na namang lumaban ngayon,” she said.
Because of her severe condition, her doctors started letting her take experimental drugs.
Because of her severe condition, her doctors started letting her take experimental drugs.
“I initially received hydroxychloroquine but then on my second day in the hospital, despite receiving such medications I still had difficulty breathing,” Fuentebella said.
“I initially received hydroxychloroquine but then on my second day in the hospital, despite receiving such medications I still had difficulty breathing,” Fuentebella said.
“My clinical status deteriorated and my medical team decided to discontinue hydroxychloroquine and started another investigational drug which are tocilizumab and lopinavir/ritonavir.”
“My clinical status deteriorated and my medical team decided to discontinue hydroxychloroquine and started another investigational drug which are tocilizumab and lopinavir/ritonavir.”
Those medicines are off-label drugs initially created for other diseases but are being tested against COVID-19. Hydroxychloroquine and lopinavir/ritonavir are among the drugs included in the World Health Organization’s multi-country clinical trials, which includes the Philippines.
Those medicines are off-label drugs initially created for other diseases but are being tested against COVID-19. Hydroxychloroquine and lopinavir/ritonavir are among the drugs included in the World Health Organization’s multi-country clinical trials, which includes the Philippines.
PLASMA THERAPY
But because her condition was not improving, her doctors decided to try convalescent plasma transfusion.
But because her condition was not improving, her doctors decided to try convalescent plasma transfusion.
It took 3 days before they found a donor who matched her blood type.
It took 3 days before they found a donor who matched her blood type.
“Three days after plasma was given, my oxygenation status improved. Eventually my chest x-rays were normal. We were not sure if it was the plasma because multiple interventions were given, but it was the immediate intervention given prior to improvement was the plasma,” Fuentebella said.
“Three days after plasma was given, my oxygenation status improved. Eventually my chest x-rays were normal. We were not sure if it was the plasma because multiple interventions were given, but it was the immediate intervention given prior to improvement was the plasma,” Fuentebella said.
By Monday, 3 weeks since she first experienced symptoms for COVID-19, Fuentebella was already feeling well and was just waiting for the results of her test. She had also just celebrated her 27th birthday at the hospital.
By Monday, 3 weeks since she first experienced symptoms for COVID-19, Fuentebella was already feeling well and was just waiting for the results of her test. She had also just celebrated her 27th birthday at the hospital.
Once she tests negative for COVID-19, she can go back to her family and undergo another 14-day home quarantine.
Once she tests negative for COVID-19, she can go back to her family and undergo another 14-day home quarantine.
Fuentebella said she wants to return to the frontlines soon but will need to recover not just physically but also mentally and spiritually.
Fuentebella said she wants to return to the frontlines soon but will need to recover not just physically but also mentally and spiritually.
She said she now looks back on her experience positively as she was able to experience first-hand what patients with severe illnesses experience.
She said she now looks back on her experience positively as she was able to experience first-hand what patients with severe illnesses experience.
“Feeling ko ibinigay ni God sa akin ’yung experience na iyon para mas maintindihan ko ’yung mga pasyente ko. Kasi pinakapinagdadasal ko sana maging magaling akong doctor. And feeling ko binigay ito sa akin ni God ’yung opportunity na maramdaman ’yun para sa future mas maalagaan ko nang mabuti ’yung mga pasyente ko,” she said.
“Feeling ko ibinigay ni God sa akin ’yung experience na iyon para mas maintindihan ko ’yung mga pasyente ko. Kasi pinakapinagdadasal ko sana maging magaling akong doctor. And feeling ko binigay ito sa akin ni God ’yung opportunity na maramdaman ’yun para sa future mas maalagaan ko nang mabuti ’yung mga pasyente ko,” she said.
(I feel that God made me go through this experience so I can understand my patients better. I always pray that I become a better doctor, and I feel like this was an opportunity that God gave me so that in the future I can better take care of my patients.)
(I feel that God made me go through this experience so I can understand my patients better. I always pray that I become a better doctor, and I feel like this was an opportunity that God gave me so that in the future I can better take care of my patients.)
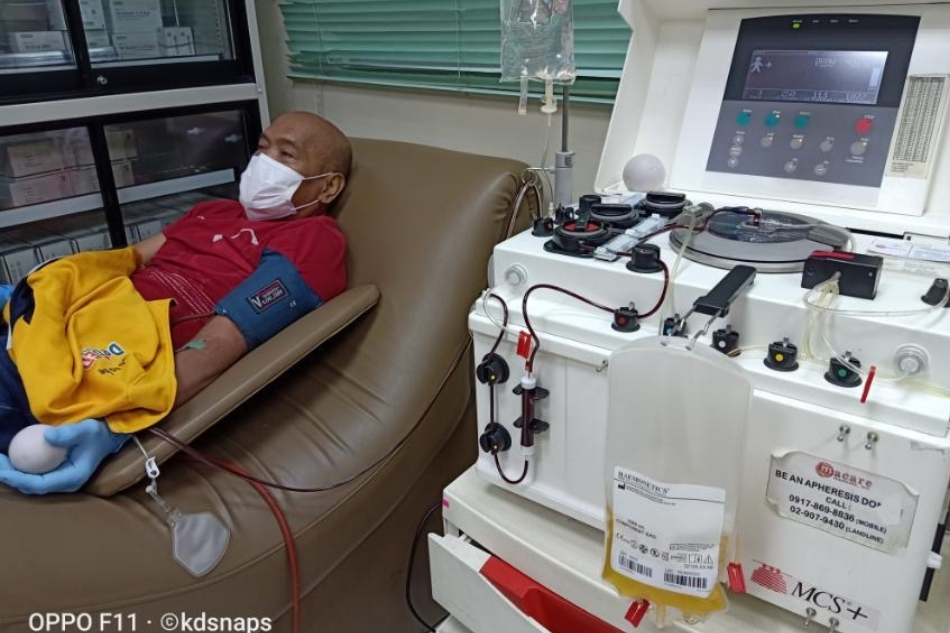
Her goal now is to convince more COVID-19 survivors to donate plasma.
Her goal now is to convince more COVID-19 survivors to donate plasma.
“It (plasma therapy) may have been what cured me. And I hope those who recovered already can help patients in critical condition like me,” she said.
“It (plasma therapy) may have been what cured me. And I hope those who recovered already can help patients in critical condition like me,” she said.
Dr. Flordeluna Zapata-Mesina, a hematologist and member of the Philippine College of Hematology and Transfusion Medicine, told ABS-CBN News that convalescent plasma is not a new treatment.
Dr. Flordeluna Zapata-Mesina, a hematologist and member of the Philippine College of Hematology and Transfusion Medicine, told ABS-CBN News that convalescent plasma is not a new treatment.
She said it has been used during other epidemics such as the Spanish Flu and the Ebola outbreak.
She said it has been used during other epidemics such as the Spanish Flu and the Ebola outbreak.
“There are also small studies from China showing its positive effect on COVID patients,” she said.
“There are also small studies from China showing its positive effect on COVID patients,” she said.
Plasma is the yellow liquid found in blood that contains antibodies. Because COVID-19 survivors have recovered from the illness, it is believed that their antibodies can help other patients fight the disease.
Plasma is the yellow liquid found in blood that contains antibodies. Because COVID-19 survivors have recovered from the illness, it is believed that their antibodies can help other patients fight the disease.
Mesina said plasma is extracted from a qualified donor then transfused into a patient.
Mesina said plasma is extracted from a qualified donor then transfused into a patient.
“Convalescent plasma may not work for all COVID-19 patients,” she explained. “There should be proper timing. It should be given before the virus has damaged any of the patient’s organs.”
“Convalescent plasma may not work for all COVID-19 patients,” she explained. “There should be proper timing. It should be given before the virus has damaged any of the patient’s organs.”
Mesina said the best time would be from Day 9 to 14 or even up to Day 21 since the patient got sick.
Mesina said the best time would be from Day 9 to 14 or even up to Day 21 since the patient got sick.
The treatment, she said, is especially helpful in severe cases.
The treatment, she said, is especially helpful in severe cases.
The WHO earlier said that a plasma transfusion can serve as a boost to the patient’s immunity.
The WHO earlier said that a plasma transfusion can serve as a boost to the patient’s immunity.
LOW ON DONORS
Unfortunately, Mesina said there are not enough donors.
Unfortunately, Mesina said there are not enough donors.
The Philippine College of Hematology and Transfusion Medicine has been calling for donors for the following hospitals:
The Philippine College of Hematology and Transfusion Medicine has been calling for donors for the following hospitals:
- Asian Hospital And Medical Center,
- Cardinal Santos Medical Center,
- Jose B. Lingad Regional Medical Center,
- Makati Medical Center,
- The Medical City,
- UST Hospital,
- UERM Memorial Medical Center.
- Asian Hospital And Medical Center,
- Cardinal Santos Medical Center,
- Jose B. Lingad Regional Medical Center,
- Makati Medical Center,
- The Medical City,
- UST Hospital,
- UERM Memorial Medical Center.
Mesina said those who are allowed to donate should show proof that they had COVID-19 and that they already tested negative. They should also not have any symptoms for the last 14 days.
Mesina said those who are allowed to donate should show proof that they had COVID-19 and that they already tested negative. They should also not have any symptoms for the last 14 days.
The same standards for blood donors will also be required: having a weight of at least 50 kilograms, having normal blood pressure and blood sugar and not having any illness such as hepatitis or HIV.
The same standards for blood donors will also be required: having a weight of at least 50 kilograms, having normal blood pressure and blood sugar and not having any illness such as hepatitis or HIV.
Mesina assured the public that donors will undergo thorough screening to ensure that their blood is safe.
Mesina assured the public that donors will undergo thorough screening to ensure that their blood is safe.
For now, experts use fresh plasma donations so they are also calling on local government units to assist in transporting the substance. The same goes for regular blood donations, which she said has drastically done down.
For now, experts use fresh plasma donations so they are also calling on local government units to assist in transporting the substance. The same goes for regular blood donations, which she said has drastically done down.
“We think the reason why we have a low blood donation rate is because of the quarantine. Not all of our donors have vehicles. If the LGUs can offer free rides for blood donors that would be helpful,” Mesina said.
“We think the reason why we have a low blood donation rate is because of the quarantine. Not all of our donors have vehicles. If the LGUs can offer free rides for blood donors that would be helpful,” Mesina said.
The doctor said the only negative effect of the treatment are allergies from the blood transfusion or the very rare occurrence of acute lung injury, the latter mostly occurring when the receiving patient is elderly, high risk or have pre-existing medical conditions.
The doctor said the only negative effect of the treatment are allergies from the blood transfusion or the very rare occurrence of acute lung injury, the latter mostly occurring when the receiving patient is elderly, high risk or have pre-existing medical conditions.
Patients are always asked for their informed consent before receiving the treatment.
Patients are always asked for their informed consent before receiving the treatment.
COVID-19 survivors who want to donate plasma may contact the hospitals’ blood banks through the following numbers:
COVID-19 survivors who want to donate plasma may contact the hospitals’ blood banks through the following numbers:
- Asian Hospital And Medical Center (02)8 771 9000 loc 5789 or 0917 8048587
- Cardinal Santos Medical Center - (02)8 727 0001 loc 4105
- Jose B. Lingad Regional Medical Center - (045) 9613363
- Makati Medical Center - (02)8 888 8999 loc 3016
- The Medical City - (02)8 988 1000 loc 6108
- UERM Memorial Medical Center - (02)8 751 0861 loc 235
- UST Hospital - (02)8 731 3001 loc 2395
- Asian Hospital And Medical Center (02)8 771 9000 loc 5789 or 0917 8048587
- Cardinal Santos Medical Center - (02)8 727 0001 loc 4105
- Jose B. Lingad Regional Medical Center - (045) 9613363
- Makati Medical Center - (02)8 888 8999 loc 3016
- The Medical City - (02)8 988 1000 loc 6108
- UERM Memorial Medical Center - (02)8 751 0861 loc 235
- UST Hospital - (02)8 731 3001 loc 2395
They may also reach the PCHTMC Facebook Page for more details.
They may also reach the PCHTMC Facebook Page for more details.
ADVERTISEMENT
ADVERTISEMENT