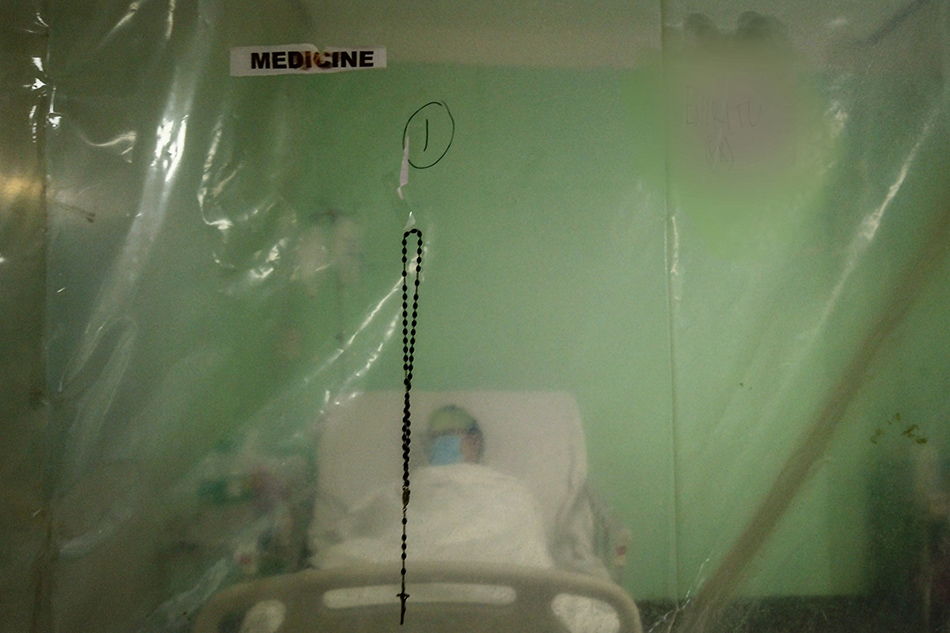
'4-6 dead on arrival daily': Ospital ng Maynila overwhelmed by COVID-19 patients
ADVERTISEMENT

Welcome, Kapamilya! We use cookies to improve your browsing experience. Continuing to use this site means you agree to our use of cookies. Tell me more!
'4-6 dead on arrival daily': Ospital ng Maynila overwhelmed by COVID-19 patients
Chiara Zambrano,
ABS-CBN News
Published Jul 31, 2020 08:02 AM PHT
|
Updated Jul 31, 2020 03:40 PM PHT
"We see four to six DOAs (Dead on Arrival) in a day."
"We see four to six DOAs (Dead on Arrival) in a day."
Yet another Metro Manila hospital has been forced to temporarily close its doors to new patients after being overwhelmed by COVID-19.
Yet another Metro Manila hospital has been forced to temporarily close its doors to new patients after being overwhelmed by COVID-19.
From today, July 31, until August 9, Ospital ng Maynila will no longer accept incoming patients, and retain only the patients already in their care. The hospital cited two reasons: their beds are full, and the virus has begun to spread across the different departments of the hospital.
From today, July 31, until August 9, Ospital ng Maynila will no longer accept incoming patients, and retain only the patients already in their care. The hospital cited two reasons: their beds are full, and the virus has begun to spread across the different departments of the hospital.
The 25 beds allotted for COVID-19 patients are now occupied and have been for a while. New patients, meanwhile, keep coming, asking to be treated.
The 25 beds allotted for COVID-19 patients are now occupied and have been for a while. New patients, meanwhile, keep coming, asking to be treated.
ADVERTISEMENT
Doctor Karen Kaye Uy, the hospital’s chief resident for internal medicine, said the surge started in June, and spiked late July as a result of the loosening of Metro Manila’s lockdown measures.
Doctor Karen Kaye Uy, the hospital’s chief resident for internal medicine, said the surge started in June, and spiked late July as a result of the loosening of Metro Manila’s lockdown measures.
"Malala itong pagpasok ng last 2 weeks ng July,” Uy said. “Maya-maya talaga, as in maraming patients na dumadating na with respiratory symptoms.”
"Malala itong pagpasok ng last 2 weeks ng July,” Uy said. “Maya-maya talaga, as in maraming patients na dumadating na with respiratory symptoms.”
[The last 2 weeks of July have been the worst. Every so often, another patient comes in, many of them with respiratory symptoms.]
[The last 2 weeks of July have been the worst. Every so often, another patient comes in, many of them with respiratory symptoms.]
What’s worse, Uy said, is that not all patients brought to the hospital are even still alive, painting a picture of the grim situation other Metro Manila hospitals are in.
What’s worse, Uy said, is that not all patients brought to the hospital are even still alive, painting a picture of the grim situation other Metro Manila hospitals are in.
“We’re seeing a lot of DOA (dead on arrival) lately. Nitong mga duty namin nitong nakaraan, we get to have four to six DOAs in a duty,” said Uy.
“We’re seeing a lot of DOA (dead on arrival) lately. Nitong mga duty namin nitong nakaraan, we get to have four to six DOAs in a duty,” said Uy.
ADVERTISEMENT
"May mga patients na they come in from other hospitals, desaturated na but they still opted to transfer kasi nakikita nila sobrang haba ng pila, sobrang dami ng patients. And then when they come in, 'yon, DOA na. Patients na matatanda, naka-swero, galing din sa ibang ospital a few days ago but they opted to go home kasi wala nang vacancy.”
"May mga patients na they come in from other hospitals, desaturated na but they still opted to transfer kasi nakikita nila sobrang haba ng pila, sobrang dami ng patients. And then when they come in, 'yon, DOA na. Patients na matatanda, naka-swero, galing din sa ibang ospital a few days ago but they opted to go home kasi wala nang vacancy.”
[We’re seeing a lot of DOA (dead on arrival)s lately. In our last several shifts, we get to have four to six DOAs in a duty. They’re patients who come in from other hospitals. They’re desaturated but they still opted to transfer because they saw that the lines were already too long, the patients too many. And then when they come in, there. they’re already DOA. These are elderly patients, patients with IVs, who came from other hospitals but opted to go home because there was no vacancy.]
[We’re seeing a lot of DOA (dead on arrival)s lately. In our last several shifts, we get to have four to six DOAs in a duty. They’re patients who come in from other hospitals. They’re desaturated but they still opted to transfer because they saw that the lines were already too long, the patients too many. And then when they come in, there. they’re already DOA. These are elderly patients, patients with IVs, who came from other hospitals but opted to go home because there was no vacancy.]
Ospital ng Maynila has set up makeshift tents as additional spaces for patients but even these are not enough, said Doctor Karl Laqui, the OIC Director.
Ospital ng Maynila has set up makeshift tents as additional spaces for patients but even these are not enough, said Doctor Karl Laqui, the OIC Director.
"Ang mahirap sa lahat is 'yung tumanggi eh. Yung sabihing 'puno na ho kami,'" Laqui said. "Sasabihin sa'yo nung pasyente pagdating dito, 'Pang-anim na ho namin kayong ospital, ano ba hong magagawa ninyo, paano niyo ho kami matutulungan?'"
"Ang mahirap sa lahat is 'yung tumanggi eh. Yung sabihing 'puno na ho kami,'" Laqui said. "Sasabihin sa'yo nung pasyente pagdating dito, 'Pang-anim na ho namin kayong ospital, ano ba hong magagawa ninyo, paano niyo ho kami matutulungan?'"
[The most difficult thing to do is to refuse a patient. To be forced to say, ‘We’re already full.’ When they arrive, the patients tell us things like ‘You are the sixth hospital I’ve tried, can you help me?’]
[The most difficult thing to do is to refuse a patient. To be forced to say, ‘We’re already full.’ When they arrive, the patients tell us things like ‘You are the sixth hospital I’ve tried, can you help me?’]
ADVERTISEMENT
Laqui said the situation is taking an emotional toll on the hospital’s younger health workers, who have been fighting to treat as many ill patients as they can.
Laqui said the situation is taking an emotional toll on the hospital’s younger health workers, who have been fighting to treat as many ill patients as they can.
"Our residents, they’re young doctors. Siyempre idealistic sila. Ang ideal nila is really to help everybody and to cure everybody. So they have a dilemma on what to do. They cannot just admit them kasi wala namang space. But they also cannot turn them away. Kaya we’re forced to have 'yung tents namin dito. Mahirap.”
"Our residents, they’re young doctors. Siyempre idealistic sila. Ang ideal nila is really to help everybody and to cure everybody. So they have a dilemma on what to do. They cannot just admit them kasi wala namang space. But they also cannot turn them away. Kaya we’re forced to have 'yung tents namin dito. Mahirap.”
[“Our residents, they’re young doctors. Of course they’re idealistic. Their ideal is really to help everybody and to cure everybody. So they have a dilemma on what to do. They cannot just admit them because there’s no more space. But they also cannot turn them away. That’s why we’re forced to have those tents there. It’s difficult.]
[“Our residents, they’re young doctors. Of course they’re idealistic. Their ideal is really to help everybody and to cure everybody. So they have a dilemma on what to do. They cannot just admit them because there’s no more space. But they also cannot turn them away. That’s why we’re forced to have those tents there. It’s difficult.]
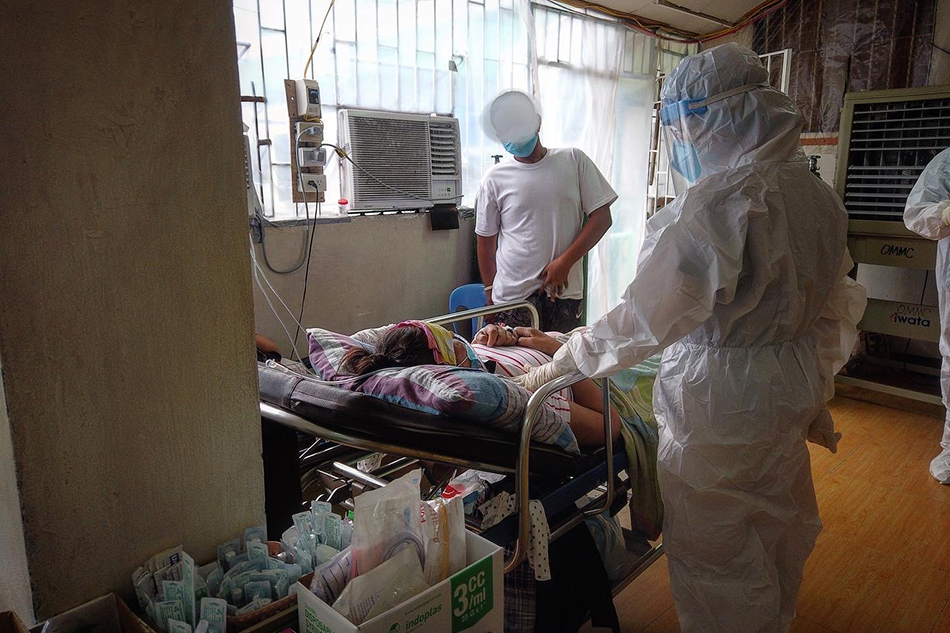
Outside the building, an old room beside the parking lot has been converted into a makeshift ward for patients, too. Nine patients awaiting results of their COVID-19 tests as well as their companions share the same space without barriers, with only a few electric fans to alleviate the stuffiness in the air. One patient – a woman – was lying calmly while her daughter – a teacher – was holding a virtual class by her bedside. Right beside her was a companion of an elderly man in diapers. In another corner, another patient sat beside his oxygen tank. Dr. Uy tried to wake up another female patient by the door, but got little response.
Outside the building, an old room beside the parking lot has been converted into a makeshift ward for patients, too. Nine patients awaiting results of their COVID-19 tests as well as their companions share the same space without barriers, with only a few electric fans to alleviate the stuffiness in the air. One patient – a woman – was lying calmly while her daughter – a teacher – was holding a virtual class by her bedside. Right beside her was a companion of an elderly man in diapers. In another corner, another patient sat beside his oxygen tank. Dr. Uy tried to wake up another female patient by the door, but got little response.
"Malaki na ang in-improve niya," Uy said of the woman. Nakakadilat na siya ngayon."
"Malaki na ang in-improve niya," Uy said of the woman. Nakakadilat na siya ngayon."
ADVERTISEMENT
[She’s improved a lot. She can open her eyes now.]
[She’s improved a lot. She can open her eyes now.]
Both Uy and Laqui recognize that the makeshift facilities are far from ideal. But nothing has been ideal for awhile.
Both Uy and Laqui recognize that the makeshift facilities are far from ideal. But nothing has been ideal for awhile.
"Hindi siya yung best conditions. But it’s better than nothing," said Laqui. "Kahit sabihin mong spartan yung area, it’s best pa rin na nandidito sila, and they have a doctor to provide them the medical na pangangailangan nila."
"Hindi siya yung best conditions. But it’s better than nothing," said Laqui. "Kahit sabihin mong spartan yung area, it’s best pa rin na nandidito sila, and they have a doctor to provide them the medical na pangangailangan nila."
[These aren’t the best conditions. But it’s better than nothing. Even if you say the area is spartan, it’s still the best because they have doctors here to provide them their medical needs.]
[These aren’t the best conditions. But it’s better than nothing. Even if you say the area is spartan, it’s still the best because they have doctors here to provide them their medical needs.]
'The virus has spread across different departments'
Apart from the hospital reaching full capacity, the reason why Dr. Laqui was compelled to write City Hall and request for the temporary closure is because the virus has begun to spread among hospital staff – even those who don’t even deal directly with patients.
Apart from the hospital reaching full capacity, the reason why Dr. Laqui was compelled to write City Hall and request for the temporary closure is because the virus has begun to spread among hospital staff – even those who don’t even deal directly with patients.
ADVERTISEMENT
"May personnel kami na supposedly hindi dapat magpa-positive kasi wala naman silang contact sa pasyente," Laqui said. "Sa OB, meron kami. Sa surgery, meron kami. Sa billing, meron kami. Sa engineering, meron kami. Parang tingin namin, it’s no longer na 'yung patient ang nakaka-infect sa mga personnel. Personnel to personnel na 'yung spread ng infection, which is very scary, considering kung mangyayari 'yon, we’ll be left with no personnel to take care of our patients."
"May personnel kami na supposedly hindi dapat magpa-positive kasi wala naman silang contact sa pasyente," Laqui said. "Sa OB, meron kami. Sa surgery, meron kami. Sa billing, meron kami. Sa engineering, meron kami. Parang tingin namin, it’s no longer na 'yung patient ang nakaka-infect sa mga personnel. Personnel to personnel na 'yung spread ng infection, which is very scary, considering kung mangyayari 'yon, we’ll be left with no personnel to take care of our patients."
[We have personnel that supposedly shouldn’t test positive because they have no contact with the patients. We have personnel infected in OB. We have personnel infected in surgery. We have personnel infected in billing. We have personnel infected in engineering. We now believe it’s no longer the patients infecting the personnel. The infection is spreading from personnel to personnel, which os very scary, considering if it happens, we’ll be left with no personnel to take care of our patients.]
[We have personnel that supposedly shouldn’t test positive because they have no contact with the patients. We have personnel infected in OB. We have personnel infected in surgery. We have personnel infected in billing. We have personnel infected in engineering. We now believe it’s no longer the patients infecting the personnel. The infection is spreading from personnel to personnel, which os very scary, considering if it happens, we’ll be left with no personnel to take care of our patients.]
Eleven of the 25 confirmed COVID-19 patients confined to Ospital ng Maynila are their very own personnel. Another four personnel with the virus are on home quarantine. Thirty two other symptomatic personnel are quarantined at home awaiting their test results. Fifty eight other people have been identified as close contacts.
Eleven of the 25 confirmed COVID-19 patients confined to Ospital ng Maynila are their very own personnel. Another four personnel with the virus are on home quarantine. Thirty two other symptomatic personnel are quarantined at home awaiting their test results. Fifty eight other people have been identified as close contacts.
"We have one department – ophthalmology – doctors nila are seven. Six of them are symptomatic na, although they’re awaiting yung result. It’s very unusual na mangyari. Another one would be pathology. Sa pathology, wala silang contact sa pasyente na close, 'yung defined na contact ng DOH. Pero three na doctors na nila ang nag-positive. And some of them are symptomatic na," Lagui said.
"We have one department – ophthalmology – doctors nila are seven. Six of them are symptomatic na, although they’re awaiting yung result. It’s very unusual na mangyari. Another one would be pathology. Sa pathology, wala silang contact sa pasyente na close, 'yung defined na contact ng DOH. Pero three na doctors na nila ang nag-positive. And some of them are symptomatic na," Lagui said.
[We have one department – ophthalmology – they have seven doctors. Six of them are already symptomatic, although they’re awaiting their results. It’s very unusual. Another one would be pathology. They have no close contacts with patients – at least by the definition of the Department of Health. But three doctors there have tested positive. Some of them have symptoms already.]
[We have one department – ophthalmology – they have seven doctors. Six of them are already symptomatic, although they’re awaiting their results. It’s very unusual. Another one would be pathology. They have no close contacts with patients – at least by the definition of the Department of Health. But three doctors there have tested positive. Some of them have symptoms already.]
ADVERTISEMENT
Seeing coworkers hit by COVID-19 is certainly unsettling for Dr. Uy.
“Once you see them kasi, it’s different. For one, you’ve known them for a long time already. And then your own fear also sets in. you get to ask yourself, what if I get to see myself in his shoes one day?”
Seeing coworkers hit by COVID-19 is certainly unsettling for Dr. Uy.
“Once you see them kasi, it’s different. For one, you’ve known them for a long time already. And then your own fear also sets in. you get to ask yourself, what if I get to see myself in his shoes one day?”
Uy said this is the worst state that she has seen Metro Manila in since COVID-19 hit the country. She echoes the call of other health care workers for government to place Metro Manila back under Enhanced Community Quarantine (ECQ) before the health care system loses all control.
Uy said this is the worst state that she has seen Metro Manila in since COVID-19 hit the country. She echoes the call of other health care workers for government to place Metro Manila back under Enhanced Community Quarantine (ECQ) before the health care system loses all control.
“Ngayon lang ito, na ganito talaga siya. That’s why I think a lot of doctors and health care workers are already calling for another ECQ. Kasi sobrang nao-overwhelm na 'yung healthcare system natin. And the healthcare personnel themselves are already getting infected. So who is going take care of the patients? The numbers aren’t going down, they’re only increasing, getting higher. Everyday. We need to do something,” she said.
“Ngayon lang ito, na ganito talaga siya. That’s why I think a lot of doctors and health care workers are already calling for another ECQ. Kasi sobrang nao-overwhelm na 'yung healthcare system natin. And the healthcare personnel themselves are already getting infected. So who is going take care of the patients? The numbers aren’t going down, they’re only increasing, getting higher. Everyday. We need to do something,” she said.
[We’re only seeing this now. That’s why I think a lot of doctors and health care workers are already calling for another ECQ. Our healthcare system is already being overwhelmed. And the healthcare personnel themselves are already getting infected. So who is going take care of the patients? The numbers aren’t going down, they’re only increasing, getting higher. Everyday. We need to do something.]
[We’re only seeing this now. That’s why I think a lot of doctors and health care workers are already calling for another ECQ. Our healthcare system is already being overwhelmed. And the healthcare personnel themselves are already getting infected. So who is going take care of the patients? The numbers aren’t going down, they’re only increasing, getting higher. Everyday. We need to do something.]
ADVERTISEMENT
ADVERTISEMENT